As NICUs have become more effective, any proportional incremental improvements will necessarily get smaller, so larger and larger datasets will be needed to show any trends. The NICHD has just published data about survival and major acute morbidities among extremely preterm infants, going back to 1993, and ending in 2012.
The population was infants born at 22 to 28 weeks and 400 to 1500 g, so a few larger than average 27, 28 week infants would have been excluded.
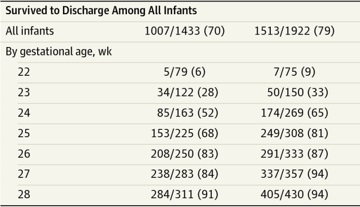
Basically there are significant upward trends in survival, and reductions in many morbidities over the entire 20 years, and continuing between 2009 and 2012. The best survival at every gestational age that they show in the table is from 2012.
This excerpt from the table shows the results from 1993 in the first column and 2012 in the second, the number in brackets is the percentage survival.
Among major morbidities, a progressive reduction in late-onset sepsis, starting in about 2006, is shown very clearly. Instead of a 34% incidence, only 24% of extremely preterm infants now have an episode of sepsis. There is a less marked but still important reduction in severe intracranial haemorrhages, from 19% to 15%, and in severe retinopathy from 13% to 11%; Most of the reduction of those 2 morbidities was in the more mature infants, and not in the 23 and 24 week babies.
But necrotizing enterocolitis hasn’t changed (it has gone up a bit from 7% to 10%), and bronchopulmonary dysplasia is increasing (from 32% to 45%). Roger Soll has written an editorial to accompany this publication. As usual I cannot argue with anything he says.
Except for one thing, he suggests that there is no breakthrough therapy on the horizon that is likely to change these morbidities. One simple breakthrough therapy that has been shown effective, but is still underused, is already with us. Widespread us of probiotics could reverse that minor trend to more NEC and lead to somewhere around a 50% reduction in NEC.
As he notes, the reduction in late-onset sepsis has followed the introduction of quality control initiatives, which treat an invasive infection as a failure, rather than inevitable. We need to do the same thing for our other morbidities.
Retinopathy is associated with poor early postnatal growth. Improving nutrition will likely reduce the incidence.
Gentle ventilation, and more non-invasive ventilation, have not yet led to the reduction in lung injury that we might have hoped, the details of exactly how we do CPAP and non-invasive ventilation, improved nursing and RT procedures, improved CPAP interfaces, and methods for detecting and avoiding lung overdistension (mostly during invasive ventilation) are needed. They are needed much more, I think, than adding another ventilatory mode that few people really understand to our latest ventilators.
One change associated with BPD however, has been a reduction in the use of postnatal steroids. As steroids reduce oxygen requirements, it may be that reducing steroid use has led to more babies being in oxygen at 36 weeks, and therefore more having a diagnosis of BPD. Which is not necessarily a bad thing in that context. Steroids have never been shown to improve lung repair, or to improve long-term pulmonary outcomes, so an increase in the somewhat artificial diagnosis of BPD may not reflect worse pulmonary outcomes in the long-term.
Those would be my prescriptions for further improving survival without morbidities: improving nutrition, improving how we do non-invasive and invasive ventilation, and universal use of probiotics.








