A great deal of time and effort is expended to detect and treat low blood sugars in the newborn. Studies to determine risk factors, monitoring schedules, and treatment strategies have taken a great deal of effort, and implementing the recommended protocols requires much effort, resources, and often separates healthy babies from their families, or at least makes them think the baby is sick. The whole point of all this is to prevent brain injury from hypoglycaemia, with the underlying premise that low blood sugars, below a certain threshold, may cause damage which will have an impact on the baby’s future, therefore it is important to detect and immediately treat the phenomenon.
Two new publications from studies co-ordinated by the Auckland group continue to challenge some of our assumptions.
The hPOD trial (Harding JE, et al. Evaluation of oral dextrose gel for prevention of neonatal hypoglycemia (hPOD): A multicenter, double-blind randomized controlled trial. PLoS Med. 2021;18(1):e1003411) showed that you could reduce the incidence of hypoglycaemia with prophylactic oral dextrose gel; that was a multicentre RCT of over 2000 newborns who were in at-risk groups. 42% of the control group developed a blood sugar under 2.6 mmol/L, compared to 37% of the treated babies. There wasn’t much effect on “severe hypoglycaemia” (<2.0) however, 9.9% vs 9.3%, on on NICU admission, which was the primary outcome variable, 9.4% vs 10.4%. At 2 years the New Zealand cohort from the study had follow up testing, 88% of them completed the assessment, a truly remarkable achievement after a short-term trial in otherwise healthy babies! (Edwards T, et al. Prophylactic Oral Dextrose Gel and Neurosensory Impairment at 2-Year Follow-up of Participants in the hPOD Randomized Trial. JAMA. 2022;327(12):1149-57). This is the table with the main results:
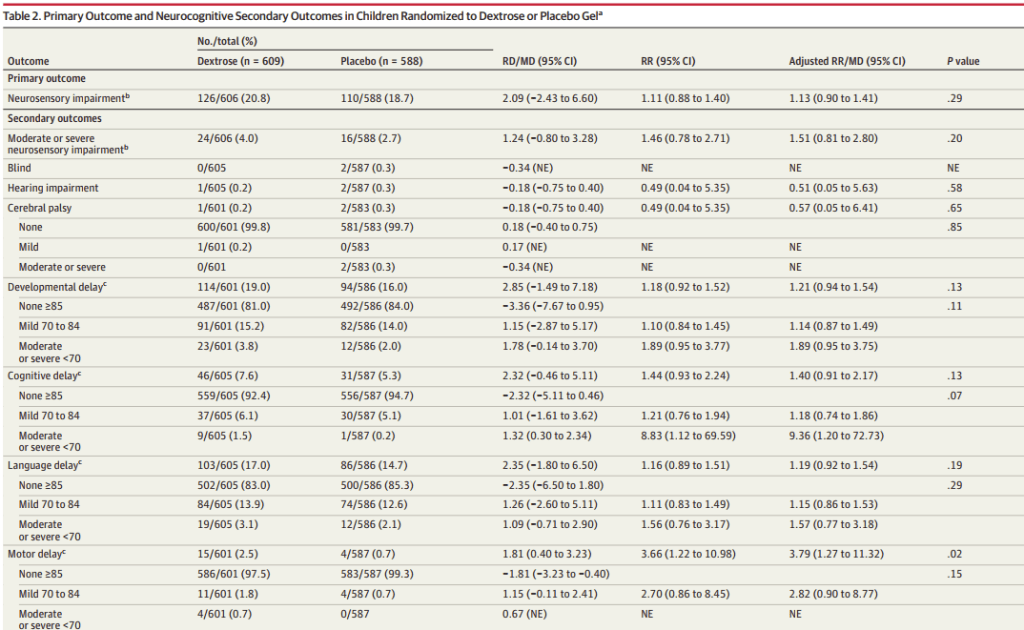
The small differences in outcome are all in favour of the placebo group. With, in particular, motor delay being more common in the dextrose group, 2.5% compared to 0.7%.
The average scores on each composite of the BayleyIII scores were higher in the placebo group, and, although the differences were very small, some of the 95% compatibility intervals for the unadjusted and adjusted mean differences did not include 0.

There were also tests of executive function which showed practically identical results in the 2 groups. On other words, no advantage at all, and some hints of an adverse impact of the oral gel when used as prophylaxis.
The other publication is from the CHYLD team, (Shah R, et al. Association of Neonatal Hypoglycemia With Academic Performance in Mid-Childhood. JAMA. 2022;327(12):1158-70). This is an evaluation of academic achievement in 480 infants from a prospective cohort, at 9 to 10 years after enrolment, which is 82% of the potentially eligible children. The children had initially been participants in either the BABIES study or SUGAR-BABIES: BABIES was a prospective cohort study of EEG monitoring in neonates at risk of hypoglycaemia, which showed no impact of hypoglycaemia on EEG activity; SUGAR-BABIES was the randomized trial of oral glucose gel as treatment for hypoglycaemia, which showed that the intervention was effective as treatment. Previous publications at 2 years showed no apparent impact of hypoglycaemia, whereas at 4.5 years there was some evidence of an association between hypoglycaemia and poor executive function. To recall in the 4.5 year follow up there were no differences in neurological outcomes or on Wechsler full scale IQ, and mean executive function scores were practically identical in the 2 groups, 13.5 (SD 6) compared to 13.3 (SD 5.7), but there was an excess of babies with scores more than 1.5 SD below the mean, 11% vs 5%, suggesting a slightly skewed distribution with an excess of lower scores in the hypoglycaemic group.
These 4.5 year findings reinforced the importance of performing this new evaluation at 9 to 10 years. Academic achievement, executive function, visual-motor integration, motor function, visual processing and behavioural problems were evaluated. No differences were found between infants with hypoglycaemia (either one blood glucose <2.6 mM/L (47 mg/dl) or an interstitial glucose <2.6 for over 10 minutes) and those who never had documented hypoglycaemia.
The differences in outcomes were small, with minor differences generally favouring the hypoglycaemia group, the only outcome for which compatibility intervals did not include no difference was the teachers evaluation of reading ability, that also favoured the hypoglycaemia children. They also evaluated the subgroup with severe (<2.0 mM/L (37 mg/dl)) or recurrent (3 or more) hypoglycaemia, and the subgroup with recurrent hypoglycaemia (3 or more episodes). None of the results look different from non-hypoglycaemic children. Here is the first part of the first results table:
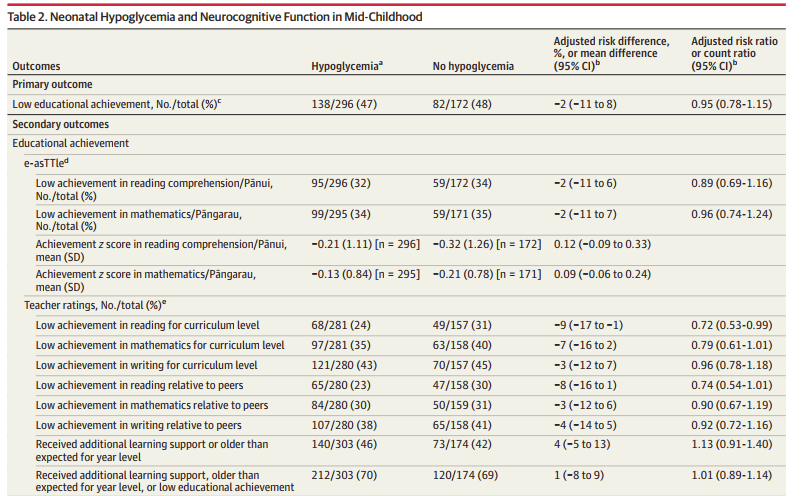
What is somewhat surprising, is how frequent low educational achievement was in all of the groups, with almost half of all the participants being “below the normative curriculum level” or “well below”, below seems to mean that they were operating at a level at least 1 year behind their peers, and well below means more than 2 years behind. This isn’t totally clear in the publication, but the statistical analysis plan in the supplement defines “below” as performing at a level 4 to 7 school terms below the peer group and, according to Google, each school year in New Zealand consists of 4 terms. “Well below” is defined as performing at a level 8 or more terms behind the school year and term norms.
The power calculations were based on the prediction that 20% of children would have this outcome. Poor educational achievement was therefore very frequent in all groups, and more than twice as frequent as expected, even though achievement was not affected by whether the children had actually developed hypoglycaemia or not.
It seems therefore likely, that the same factors that lead to an increase in risk of hypoglycaemia also lead to an increased risk of poor academic performance, and also poor outcomes in visual-motor integration, executive function and behavioural domains. These findings emphasize the need for control groups in studies of long term potential impacts of hypoglycaemia to be babies with the same profile of risk factors, but who did not develop hypoglycaemia. That has not always been the case and may have misled us as to the importance of hypoglycaemia. Obviously, if you compare at-risk babies who develop hypoglycaemia to the general population, then they would seem to have much worse outcomes. It appears that being small for gestational age or an infant of a diabetic mother, and late preterm birth are risk factors for poor outcomes on the variables that were studied. There is also a question about the background frequency of social deprivation, and the population appears a little more deprived than the general NZ population, with about 40% of the participants’ families being in the most deprived 3 deciles (it should of course be 30%), but that doesn’t to seem to me to be a big enough finding to explain most of the results.
The most dramatic interpretation of these data would be that hypoglycaemia, to <2.6 or even <2.0 mM/l is unimportant in the transitional period. Single episodes or even multiple episodes below these thresholds don’t seem to increase risk of poor outcomes, over and above just being in an at-risk group. One possible explanation of the results could have been that we miss a lot of hypoglycaemia events, and the poor outcomes might be due to undetected hypoglycaemia. However, many of the children in CHYLD had continuous interstitial glucose measurements performed and the analysis, presented in the supplement, of only babies with continuous monitoring also showed that babies who were continuously normo-glycaemic had identical poor outcomes to those with documented hypoglycaemia, and to those with hypoglycaemia during their continuous monitoring period, 48% of normo-glycaemic infants having poor educational achievement.
These data suggest that we should maybe focus on detecting and treating more severe and prolonged hypoglycaemia. It has already been shown that using 2.0 as a limit rather than 2.6 mM/l (36 rather than 47 mg/dl) does not affect long term outcomes, these new data imply that even 2.0 is too high a threshold, using dextrose gel as prophylaxis actually slightly worsened outcomes compared to placebo, and babies with documented hypoglycaemia actually did slightly better than normoglycaemic infants.
Could it be that all our screening and interventions for mild and moderate hypoglycaemia in term and near term babies are actually making things worse? Is there any way of predicting which babies are at risk of more severe hypoglycaemia? What threshold of hypoglycaemia is associated with worse outcomes? Does treating hypoglycaemia when it fall below that threshold improve outcomes? Is it possible to focus prophylaxis to prevent more severe hypoglycaemia? If so, does that improve outcomes?
And for our obstetric colleagues, can we prevent gestational diabetes, intra-uterine growth restriction, excessive intra-uterine growth, and late preterm delivery? If so, does that improve long term outcomes of these babies?
So many questions, so few answers.









Pingback: Antenatal steroids prior to late preterm delivery; still many questions, but a major shift in practice. | Neonatal Research
Hi Keith, I fully agree with your views on this topic…if the underlying premise is inadequately supported and the foundation is weak, all the guidelines are attempts to fix a number rather than solve a problem. Well stated!
Pingback: Is glucose gel safe? Is it necessary? | Neonatal Research