This blog is a bit different: not a review of a recent publication, but rather a teaching point for my junior trainees (and maybe some seniors).
The question is this: when you have preterm infant with typical HMD and respiratory distress in the first few hours of life to whom you give surfactant; what happens to pulmonary compliance? Try not to look at the answer until your knee has jerked and you have made your choice.
The correct answer is not it increases but ‘it depends’ (that is often the correct answer) but on what?
If you answered it depends on whether you are referring to static or dynamic compliance, then you clearly have either some insight into pulmonary physiology, or you made a lucky guess. Let me explain a bit more:
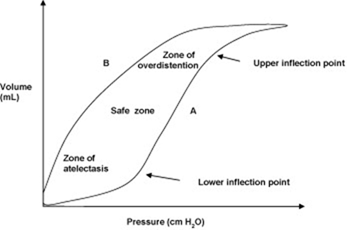
Static compliance is measured when there is no gas flow (hence static) and to produce the complete pressure volume loop the applied pressure should be taken down to zero. This gives the typical curve with its hysteresis.
When you look at the display on a modern neonatal ventilator what you see is nothing like the curve shown above, what you see looks more like a dynamic pressure-volume curve (of course it does, that is what it is!)
Dynamic compliance is measured during tidal breathing (or tidal ventilation) so delays in gas movement as a result of airway (or endotracheal tube) resistance are important, and the curves look quite different.
The dynamic Pressure-Volume Curve looks like this

-
The usual effect of giving surfactant is an improvement of STATIC lung compliance. (Stenson BJ, Glover RM, Parry GJ, Wilkie RA, Laing IA, Tarnow-Mordi WO: Static respiratory compliance in the newborn. III: Early changes after exogenous surfactant treatment. Arch Dis Child Fetal Neonatal Ed 1994, 70(1):F19-24. http://fn.bmj.com/content/70/1/F19.long)
- Now if static compliance is improved: and you make no changes on the ventilator, that is you have the same PEEP, then end-expiratory lung volume is higher.
- This shifts the lung up the pressure-volume curve, and the end-inspiratory portion is likely to be on a flatter part of the curve
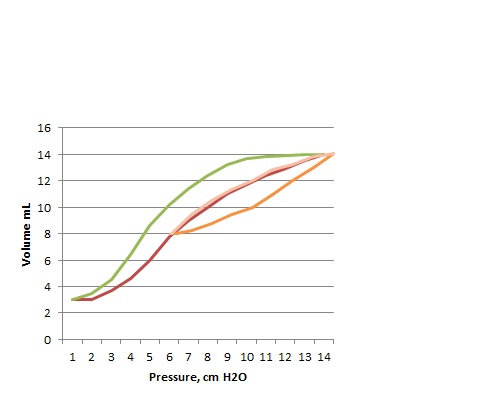
A before and after look at Static compliance loops during surfactant treatment look like this:
BEFORE, An applied pressure increasing from 0 to 13 cmH2O gives a volume of 8 mL.
CLstat = 8mL/13 cm H2O before surfactant: 0.66 mL/cmH2O
AFTER, An applied pressure increasing from 0 to 13 cmH2O gives a volume of 11 mL
CLstat = 11mL/13 cm H2O after surfactant: 0.85 mL/cmH20
But during tidal ventilation what we see and measure are DYNAMIC loops, such as these before and after loops below.
If you look at the pressure volume loops on the front of your new fancy ventilator, that cost an extra 10,000 dollars for you to have pressure volume loops displayed, they will look like this, that is, there is no difference between pre and post surfactant loops. What you will also always see is that the end-expiratory lung volume is zero. Neonatal ventilator graphics reset to zero at the end of each breath, this has to be so, because of ETT leaks, if the graphics did not reset they would soon disappear off the screen.
So now we see that the Dynamic compliance CLdyn is 6 mL/8 cmH2O both before and after surfactant.
If we superimpose these dynamic loops on the same static curves that I constructed above you can see what has happened:
The first is Pre-surfactant:
The end-expiratory lung volume is higher, the tidal ventilation is now occurring at a higher part of the Static pressure volume relationship, and therefore at a flatter part. So if you measure dynamic compliance shortly after giving surfactant and before making any ventilator changes you see no improvement, this has been demonstrated multiple times. Here is one example of dynamic compliance before and 1 hour after surfactant therapy. (Couser R, Ferrara T, Ebert J, al. e: Effects of exogenous surfactant therapy on dynamic compliance during mechanical breathing in preterm infants with hyaline membrane disease. The Journal of Pediatrics 1990, 116(1):119-124. http://www.sciencedirect.com/science/article/pii/S0022347605816609)
| Surfactant | Control | |||
| Before | After | Before | After | |
| Compliance (ml/cm H20/kg) mean (SD) | 0.43 (0.21) | 0.45 (0.45) | 0.33 (0.14) | 0.33 (0.13) |
This means that you cannot use the pulmonary graphics to determine whether the PEEP is optimal or if the baby is ready to wean. A better way to determine whether the surfactant has had an effect is simply to watch the FiO2; as the figure in Ben Stenson’s article referenced above shows, the decrease in FiO2 occurs at the same time as the improvement in Static Compliance. So when the FiO2 falls, reduce the PEEP: you will immediately afterward see the pip fall (on volume ventilation) or the volume increase (on pressure ventilation), and now you will be able to note the improvement in compliance.
Infants who reduce to 21% after surfactant can be managed with a reduction in PEEP to as low as 3 cmH2O (Dimitriou G, Greenough A, Laubscher B: Appropriate positive end expiratory pressure level in surfactant-treated preterm infants. Eur J Pediatr 1999, 158:888-891 http://www.springerlink.com/content/jumq39g0c58auql7/?MUD=MP) or even to 2 cmH2O (Sandberg KL, Silberberg AR
What Is the  Best
Best Positive End Expiratory Pressure (PEEP) in Ventilated Low Birth Weight Infants? PAS-meeting abstracts 2009, #3858.115).
Positive End Expiratory Pressure (PEEP) in Ventilated Low Birth Weight Infants? PAS-meeting abstracts 2009, #3858.115).
Please don’t tell me that this is ‘below physiologic PEEP’ as many residents have told me in the past. There is no such thing as physiologic PEEP. Positive pressure ventilation is not physiologic. The physiologic pressure in the airways at the end of expiration is zero. If it were not so, it would not be the end of expiration.
So the actual optimal PEEP would be what allows airways and airspaces to stay patent, and at the same time avoids overdistension. It is unlikely that there is one pressure which will suit all babies, but PEEP which is very low can be optimal for some babies, you can tell if you have gone too low when the FiO2 starts to increase again.
So when you give surfactant, don’t expect a change in the pressure volume loops, expect the FiO2 to decrease, when this occurs decrease the PEEP, and if the baby stays in 21% you can decrease to 3 cmH2O. Then get the baby extubated!













Thanks for this extremely useful notes,but when my ventilator reads for me tidal volume that increased after surfactant ….the first thing i always do is to decrease the PIP first for fear of air leak syndrome ….. Never thought to start with PEEP.what is ur advice …..thanks again
Thank you sir, extremely helpful article, we have been reducing the PIP to reduce air leak. Sir, should we not reduce the PIP? I always reduced both FIO2 parallel with pip to reduce mismatch. PEEP was last to reduce.Would really appreciate Ur suggestion.
I don’t think your approach is wrong, if you reduce pip you will indeed reduce the end-inspiratory lung volume, which is probably most damaging to the lung. But you will of course reduce tidal volume, and risk under-ventilating the baby, while still having a lung which is overdistended at end-expiration.
I think the best approach is to have the baby on volume ventilation at a tidal volume of probably about 5 mL/kg, and reduce the PEEP according to the FiO2. THat way the pip will reduce automatically adn the overall minute ventilation will not be much affected.
If you don’t have volume ventilation you can achieve a similar result by watching the tidal voluem adn reducing the pip to achieve the Vt that you want. And if you have older ventilators that don’t measure tidal volume then watching the chest move and trying to limit the pip is a good approach.