Marcus Brecht and Dominic Wilkinson have just published an interesting study detailing treatment limitation discussions in the NICU which came after diagnosis of major CNS injury, and what happened to the babies after these discussions.
There is a lot which is of interest in this study, but I want to highlight one particular finding.
When we have such discussions with parents, it is usually because we are concerned enough about the long term outcome of the babies to consider redirection of care, from curative to comfort care. When we have these discussions about limiting or withdrawing life-sustaining interventions, sometimes the decision is to continue with active intensive care, and therefore some infants will survive. In this study the authors show what happened to the babies after the discussion, which survived, and how they did in the long term.
They showed, among those preterm babies who survived, that most of them had no impairment or only mild impairment. Now the numbers were small, but this is consistent with what I was writing about in the last post, early head ultrsound findings are very poor for prognosticaiton.
Which all makes you think… or at least it makes me think, about the others; the many babies who have had comfort care instituted because the head ultrasound looked really bad, but who, in the end would probably have been OK, either unimpaired, mildly or moderately impaired, and who would have had a good life.
Which brings me to another study, from the Pediatrix database detailing causes of death in the NICU; many deaths, of course are among very preterm infants.
The first cause of death among the very preterm was extreme prematurity (79 of the 229 deaths), which is too vague I think to be very helpful, I would have preferred it if this had been clarified, some of the most severely preterm babies develop major metabolic abnormalities and just “fall apart” in the first few days, is that what this group had? The most useful data from this study is the frequency of other diagnoses of potentially preventable complications, sepsis and acquired bowel disease, for example. Which are the third and fourth causes of death among the extremely preterm infants.
The one aetiology of neonatal death that I want to focus on for this post is the category of babies who died of Intracranial Hemorrhage. Among those 229 deaths of babies less than 25 weeks, the second most common cause of death, accounting for 33, or 14%, of the deaths, was “intracranial hemorrhage”.
In my experience death as a direct result of the physiologic consequences of IVH is actually rather rare. It certainly happens, but not very often at all.
When an infant with a severe hemorrhage has palliative care instituted, and dies afterwards, that death is often, I think, classified as being due to the hemorrhage.
I wouldn’t be surprised if most of the babies who are stated to have died of “intracranial hemorrhage” actually died after redirection of care, as a result of head ultrasound findings, which isn’t really the same as dying of intracranial hemorrhage. But I don’t think it is entirely clear in this study.
We are very poor at prognosticating in individual cases based on head imaging findings; as I discussed in a previous post the positive predictive value of most findings, especially those that we see in the first week, is less than 50%. Prediction, that is, for outcomes which themselves are not necessarily very important in terms of quality of life (usually standardized developmental testing (almost always the Bayley scales) at between 18 months and 2 years of age).
To give one example, here is figure that I might have used before in this blog (from Merhar SL, et al: Grade and laterality of intraventricular haemorrhage to predict 18-22 month neurodevelopmental outcomes in extremely low birthweight infants. Acta Paediatr 2012, 101(4):414-418.), which shows that the proportion of infants with NDI (that is neurological impairment or a low developmental score at 24 months) was higher among infants with a grade 1 intraventricular hemorrhage who had postnatal steroids and late-onset sepsis (up to 50%), than among infants with bilateral grade 4 hemorrhage who did not have either of those complications (around 35%).
This means that in the first few days of life, when the hemorrhage is discovered, the worst finding that we see (bilateral grade 4 IVH) is associated with 65% of infants having no impairment by that definition. (Unless they go on to have sepsis or need postnatal steroids, in which case the chances of not having ‘NDI’ decrease to about 25%.)
I emphasize that this does not mean that those children who do not have ‘NDI’ will have no problems, they might for example have executive function problems, or behavioural difficulties, or serious issues with mathematics at school, but it does mean that we are lousy at predicting even what is called ‘NDI’; which is of only modest association with eventual functional outcomes.
Part of the problem with the poor prediction of head ultrasounds is the way they are interpreted and the way they are classified. Interpretations are somewhat subjective and there is substantial inter-observer variation in diagnosis of various lesions. Even those lesions where there is agreement however, are subject to the problems of the classification system. A small unilateral intracerebral bleed is classified as a grade 4 hemorrhage. Massive bilateral destructive lesions are also classified as grade 4 hemorrhages. The prognostic importance of those 2 extremes must be different, but you would never know from reading our literature, as there are very few articles that have tried to characterize the extent, or the laterality of the lesions. Which is one reason why I often quote the Merhar paper when I lecture about this issue, as they have done just that, and shown, in fact overall, that a unilateral grade 4 hemorrhage has no impact on ‘NDI’ at 18 to 22 months.
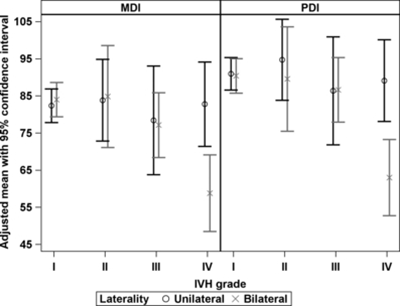
As you can see from this graph, unilateral hemorrhages of any grade do not affect the mean MDI or PDI at 18 to 22 months, only bilateral hemorrhages, are associated with a reduction in those mean scores.
Decision making in the first week of life, based head imaging findings should be avoided.










That’s a really interesting commentary. Does your post beg the question if we should bother with a screening head ultrasound at all in the first 7 to 10 days?
I do indeed think it brings the practice into question. Looking for treatable lesions, like an early ventricular dilatation after an IVH, which needs following to see if progressive dilatation develops, that might be a good reason for doing the ultrasounds.
Certainly interpreting the ultrasound in isolation for trying to predict outcomes is very unreliable.
Research has shown that poor neurodevelopmental outcome is associated with gross parenchymal lesions either hemorrhagic or ischemic leaving cystic lesions of 1 cm diameter or greater with unilateral lesions having a better prognosis than bilateral, frontal lesions doing better than occipito-parietal lesions and even then you can not always tell. Only with very large bilateral lesions can you really be certain tha it is very bad news