In response to a couple of thoughtful comments to my previous post, I thought I would try to address the specific issue of the infant of 35 weeks. (Faix RG, et al. Whole-Body Hypothermia for Neonatal Encephalopathy in Preterm Infants 33 to 35 Weeks’ Gestation: A Randomized Clinical Trial. JAMA Pediatr. 2025;179(4):396-406).
There is clearly some room for discussion, not only are obstetric estimates of gestational age uncertain, but what is the real difference between an infant at 35 weeks and 6 days, compared to 36 weeks exactly? Should we really determine therapy based on whether the baby was born before or after midnight?
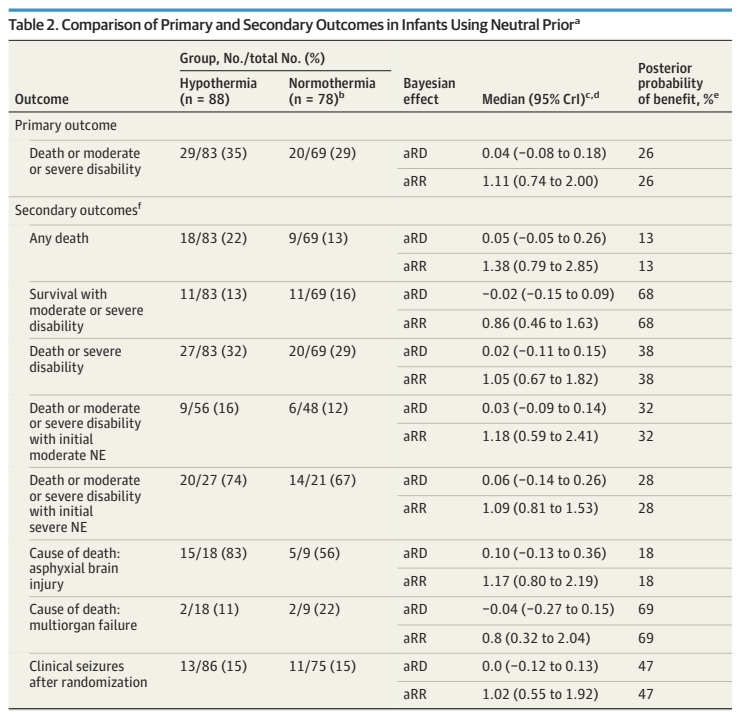
The discussion section of this new article reports on personal communication with the investigators behind the 2 previous trials that included some babies at 35 weeks gestation. Apparently, in total there were 7 babies, 2 controls (1 died and 1 survived without handicap), and 5 cooled (2 deaths, 2 survivors with disability, and 1 without). From the supplemental data supplied with the new article, there were 48 infants of 35 wk GA in this trial, 20 controls and 28 infants treated with hypothermia.
Adding all the results together gives the following :
| Control | Hypothermia | ||||
| Death | Disability | No disability | Death | Disability | No disability |
| 4 | 1 | 17 | 5 | 2 | 23 |
I performed an ad hoc Bayesian analysis myself, using an on-line calculator, which gave probabilities of close to 50% for each of the 2 options being preferable, for the combined outcome of “death or disability”, but you don’t really need to do that, there clearly is next to no difference in the outcomes.
This is, of course, an extremely limited analysis. I do not know if the definitions of disability (moderate or severe) were the same in those 2 prior trials as in the new trial, the 2 prior trials being Eicher et al and ICE. I don’t know how definite the obstetricians were in their calculation of GA, I don’t know how many babies in the various trials were lost to follow up, or if there were babies who died between discharge and follow up in the previous trials. All that said, the very limited data available do not show a major benefit of cooling at 35 weeks.
We could ask, why would therapeutic hypothermia suddenly become effective at 36 weeks 0 days? That is inherently unlikely, and I think we really need to have an Individual Patient Data meta-analysis, analysing the outcomes of the hypothermia trials by week of gestational age, the most likely outcome of such an analysis, I posit, would be a progressively greater benefit as GA advances, with perhaps harm prior to 35 weeks, no real difference between around 35 and 36 weeks, and improved survival and improved outcomes among survivors born at term. Here are the Forest plots of the results for death, and for major disability among survivors, from the latest version of the Cochrane review, which dates from 2013. CoolCap, n.neuro, TOBY, Shankaran and the NICHD trial all included babies from 36 weeks, the others were limited to at least 37 weeks GA.


That Cochrane review does not include data from more recent trials, which are largely in Lower and Middle Income countries. Those trials have been reviewed several times recently, including in a very new publication which appeared in a Supplement to “Neonatology” dealing with neonatal priorities in LMICs. You may already be aware of the HELIX trial, which really threw a spanner into the cooling machine works, it was a very important multicentre trial, from India, Bangladesh and Sri Lanka, which showed an increase in mortality with cooling. As an accompanying editorial clarifies, many of the infants were SGA, were outborn and were not transported by ambulance, many had MRI injury suggesting more chronic asphyxia. Nevertheless, overall, it looks from a complete SR/meta-analysis like there is no major benefit of Therapeutic Hypothermia in LMICs, but several single centre trials have often shown a benefit. I haven’t studied this data enough to be sure about the right approach, but many neonatologists working in LMICs do still offer hypothermia, if the conditions are right.
The reason for that little detour was just to demonstrate that hypothermia isn’t always beneficial, other studies have shown increases in mortality, as also suggested by the new late preterm trial. My conclusion is that for late preterms, there is no evidence of benefit; as gestational age increases it looks more and more likely that cooling decreases mortality and decreases disability. The exact point at which the probable harm among the preterm changes to the probable benefit at term is uncertain. It probably isn’t exactly at 36 weeks 0 days. It may well depend on other factors than purely GA, such as whether the infant is SGA, the duration of the asphyxial insult, and avoidance of excessive hypothermia, as well as perhaps the severity of the encephalopathy and the occurrence of seizures. Without knowing the impacts of those factors, it is impossible currently to select 35 week GA babies with HIE who are more likely to benefit.
I am trying to imagine what I would do tomorrow if I was asked to see a baby of 35 weeks and 5 days, who was, otherwise, a perfect candidate for cooling, with a good weight, a normal fetal heart rate trace until there was a clear sentinel event like a cord prolapse, who developed moderately severe encephalopathy and seizures at 3 hours of age. I think it is too easy to just say that it would have been OK to cool if he had been born 2 days later. On the other hand, without some sort of protocolised limits then we could cool everyone! I think, right now, I would say there is no clear evidence of benefit, and maintaining strict normothermia is the best, evidence-based approach. But I couldn’t be too angry at a colleague who had decided to cool such a baby.