There are a number of problems in neonatal care for which good evidence is lacking, and an evidence based approach is therefore not really possible. Two recent reviews highlight this problem.
The first is a systematic review of tactile stimulation for newborn infants with inadequate respiratory drive in the delivery room (Guinsburg R, et al. Tactile Stimulation in Newborn Infants With Inadequate Respiration at Birth: A Systematic Review. Pediatrics. 2022:e2021055067). I think, from years of experience, that it is likely that tactile stimulation does increase respiratory drive in some infants who are apnoeic of have poor respiratory effort in the delivery room. Indeed even many mammals do this, they vigorously lick their newborn offspring after birth, which might be to remove the membranes, at least in some animals, but may also stimulate respiration. I did a quick search to see if there is any data about this in mammals, but I found mostly just opinion.
We should be careful here, though, just because some apnoeic babies start breathing after being stimulated doesn’t mean that it was the stimulation that caused it. I am led to the idea of placebo buttons in elevators. Many elevators have a “door close” button, which often has no real function. In some places the regulations even state that door close buttons are not allowed to have any function, and they are only present because the universal design of the elevator cages has that space. Nevertheless, people press these buttons when they are in a rush, and often bash the button multiple times if the doors don’t close after the first push. Many people are convinced that the button closes the doors faster, even in places where they are not attached! I’ve done this myself; I actually, because I am a nerd, timed how long it takes the elevator doors of my usual elevator at the hospital to close without pressing the button, and it is exactly the same as when the button is pressed. It is still difficult to refrain from pushing the button when I am in a hurry, and usually the doors will then close!
Tactile stimulation could be the same, perhaps it has no actual effect, but, as most babies respiratory drive improves with time (or a decreasing pH in the respiratory centres), the apparent effect could be an illusion. Worse, it might distract resuscitators from intervening with effective manoeuvres when a baby actually needs more help.
Surely, it wouldn’t be too hard to determine if tactile stimulation actually works (i.e. leads to shorter time to adequate spontaneous respiration) and what the indications should be, and what method to use, and when to stop and proceed to more invasive techniques.
Ruth Guinsburg and colleagues new review winnowed the reliable evidence down to 2 observational studies, “the prespecified 3 primary outcomes were the establishment of spontaneous breathing without positive pressure ventilation (yes or no), time to the first spontaneous breath or crying from birth, and time to heart rate >100 beats per minute from birth”. I think those are entirely reasonable, and would be adequate justification for performing tactile stimulation if it was effective for any of those outcomes. Of the two trials they found that had some value, they could only extract somewhat reliable data from one of them, which only included preterm babies. The results suggested that perhaps endotracheal intubation was less frequent among infants who received stimulation, compared to the controls without stimulation; of course as an observational study there are biases which are impossible to eliminate.
Performing a randomized controlled trial of stimulation compared to no stimulation whatever would be difficult. I think it would be ethically acceptable if the no-stimulation group had a control intervention that was of low invasiveness and very safe, such as perhaps mask CPAP or low pressure PPV, but it would be essential to have buy-in from all the delivery room staff. In the days before we put babies in plastic bags after delivery, I used to teach that drying the baby with a towel was adequate stimulation, and if the baby was still not breathing after that, then the next steps should be performed. It was still difficult to stop other team members from flicking feet or rubbing the back yet again, and of course, it seems to be relatively harmless, as long as other procedures are also being performed.
It would probably be easier to perform an RCT comparing different methods of stimulation, foot flicking and back rubbing being the most commonly performed where I have worked. It would also be of enormous clinical significance if one was more effective than the other.
Another problem where there is a distinct lack of good evidence is the treatment of TTN (transient tachypnoea of the newborn) also sometimes known as RFLF (retained fetal lung fluid) which I prefer as being more euphonious, however, unfortunately “riflif” doesn’t work in Québec, where we treat TTNN (tachypnée transitoire du nouveau-né).
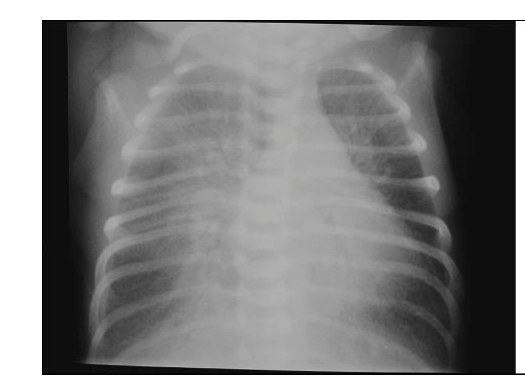
An overview of the systematic reviews of therapies for TTN has recently been published (Bruschettini M, et al. Interventions for the management of transient tachypnoea of the newborn – an overview of systematic reviews. Cochrane Database Syst Rev. 2022;2(2):CD013563). There are numerous problems in studying TTN, in part because of a lack of widely accepted diagnostic criteria, but this is an area wide open for research, for which large amounts of resources are currently used. The image above, I would suggest, is classic for TTN, but there is a great deal of inter-rater variability in the diagnosis even among radiologists.
The overview summarizes six Cochrane reviews of therapy for TTN, and the findings are disappointing. Despite the prevalence of this condition there are few studies, they all tend to be small, and the trials were mostly at high risk of bias. The largest amount of data existed for salbutamol inhalations, with 7 trials. The rationale for salbutamol is the known physiologic effect of beta adrenoreceptor stimulation on increasing lung fluid clearance, but, as endogenous circulating catecholamines are already very elevated after delivery, it is questionable whether further betamimetic stimulation would be effective or safe, the trials show low-quality evidence that tachypnoea may be shortened. For the other interventions there were between 0 and 3 trials, and no convincing evidence for the efficacy or safety of any of them.
The findings were as follows:
Salbutamol may reduce the duration of tachypnoea slightly. We are uncertain as to whether salbutamol reduces the need for mechanical ventilation. We are uncertain whether epinephrine, corticosteroids, diuretics, fluid restriction, or non‐invasive respiratory support reduce the duration of tachypnoea and the need for mechanical ventilation, due to the extremely limited evidence available. Data on harms were lacking.
I have long been sceptical of the value of CPAP and non-invasive ventilation in TTN, CPAP is great for low volume lung diseases, but lung volumes on chest x-ray of TTN are often increased (as in the radiograph above), and whether external positive pressure actually improves lung liquid clearance and clinical resolution is uncertain. This should be a research priority, shortening the duration of intensive care for these babies would benefit many thousands of families, and could save significant resources.
Currently, for apnoeic babies in the delivery room, there is no clear answer to the questions of whether we should use tactile stimulation, how, and for how long. For babies with TTN, we have no evidence-based therapy to improve the resolution of their clinical condition. Research on either of those areas has the potential to have a major impact on neonatal care.









I particularly liked the use of « winnowed » in paragraph 6. I have resolved to start using this myself.