So what about the idea of trials examining even higher oxygen saturations? Is there a chance we might further reduce mortality by aiming for saturations in the mid-90’s rather than the low 90’s?
Not so fast, even for adults that may be a really bad idea!
A fascinating systematic review, the IOTA study, was published last year in The Lancet. Chu DK, et al. Mortality and morbidity in acutely ill adults treated with liberal versus conservative oxygen therapy (IOTA): a systematic review and meta-analysis. Lancet. 2018;391(10131):1693-705. This study found 25 trials including 16,000 adults; baseline saturations were in the mid to upper 90’s in most studies, and interventions varied, but included one, liberal, group with more oxygen and a higher target saturation, and another, conservative, with more restricted oxygen use (either room air, or only when necessary, or a lower concentration as a routine compared to the liberal group). The review found a 20% increase in in-hospital mortality RR 1·21 (95% CI 1·03–1·43) with more liberal oxygen use. I remember my days, many years ago now, as an SHO (junior resident) in general internal medicine, anyone with chest pain, breathlessness, or just looking a bit peaky, would get oxygen cannulae slapped on the moment they arrived in the emergency room (or A&E as we called it). We didn’t have pulse oximeters back then in the dark ages, and didn’t want to poke everyone’s arteries for a blood gas analysis, so routine low flow oxygen was considered safe and maybe helpful. Even today, this study informs us, 34% of adults in an ambulance are given oxygen, and in the UK 15% of adults admitted to hospital are on oxygen therapy, which they may not need to maintain acceptable saturations.
IOTA also performed a meta-regression suggesting that there is a dose effect, that the higher the saturations achieved with liberal therapy the greater the adverse impact on mortality.
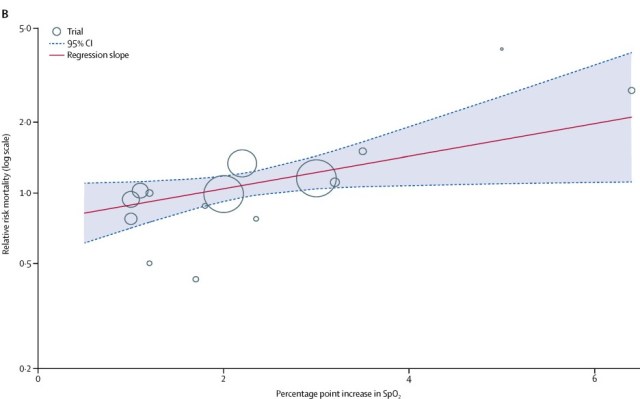
Of course adults don’t have some of the hazards that we face in neonatology, they aren’t very likely to develop retinopathy of prematurity!
Also animal models use hyperoxia in the neonatal period to create pulmonary hypertension, which can be lifelong. There are numerous examples in the literature, but here are a few, some of which note the differences, and increased sensitivity of the neonate, to the effects of hyperoxia.
(Berkelhamer SK, et al. Developmental differences in hyperoxia-induced oxidative stress and cellular responses in the murine lung. Free Radic Biol Med. 2013;61:51-60. Jimenez J, et al. Progressive Vascular Functional and Structural Damage in a Bronchopulmonary Dysplasia Model in Preterm Rabbits Exposed to Hyperoxia. Int J Mol Sci. 2016;17(10). Menon RT, et al. Long-term pulmonary and cardiovascular morbidities of neonatal hyperoxia exposure in mice. Int J Biochem Cell Biol. 2018;94:119-24. Nakanishi H, et al. Morphological characterization of pulmonary microvascular disease in bronchopulmonary dysplasia caused by hyperoxia in newborn mice. Med Mol Morphol. 2018;51(3):166-75. )
Kumar VH, et al. Neonatal hyperoxia increases airway reactivity and inflammation in adult mice. Pediatr Pulmonol. 2016;51(11):1131-41. Patel A, et al. Exposure to supplemental oxygen downregulates antioxidant enzymes and increases pulmonary arterial contractility in premature lambs. Neonatology. 2009;96(3):182-92.)
To summarize, hyperoxia is toxic to the lungs, especially in the neonatal period when antioxidant defences are reduced; in addition to oxygen free radical effects, administering excessive oxygen inhibits Guanylyl cyclase activity and increases PDE5 expression leading to increased vascular contractility and a reduced effect of nitric oxide, endogenous or exogenous. The vascular impact of these changes can lead to vascular remodelling and permanent pulmonary hypertension, as well as reduced alveolarization. Even fairly brief exposure to hyperoxia can cause some of these changes (Lakshminrusimha S, et al. Pulmonary hemodynamics in neonatal lambs resuscitated with 21%, 50%, and 100% oxygen. Pediatr Res. 2007;62(3):313-8).
In terms of clinical practice, all this reinforces the importance of preventing hyperoxia in our babies, which currently means keeping high alarm limits on whenever a baby is in oxygen and reacting when the high alarm sounds. I think in the future automated inspired oxygen controls will be very important, they now show incredible promise for reducing hyperoxia without increasing hypoxic episodes, indeed, decreasing the time being hypoxic in several studies, whether the infants were on high flow nasal cannulae (Reynolds PR, et al. Randomised cross-over study of automated oxygen control for preterm infants receiving nasal high flow. Archives of disease in childhood Fetal and neonatal edition. 2018) or ventilated (Gajdos M, et al. Effects of a new device for automated closed loop control of inspired oxygen concentration on fluctuations of arterial and different regional organ tissue oxygen saturations in preterm infants. Archives of disease in childhood Fetal and neonatal edition. 2018) or on no respiratory support other than oxygen (Zapata J, et al. A randomised controlled trial of an automated oxygen delivery algorithm for preterm neonates receiving supplemental oxygen without mechanical ventilation. Acta Paediatrica. 2014;103(9):928-33).
Not all studies show an effect on hypoxia, (Dani C. Automated control of inspired oxygen (FiO2 ) in preterm infants: Literature review. Pediatr Pulmonol. 2019;54(3):358-63), which may be partly due to apneas; if you aren’t breathing then adjusting the FiO2 is unlikely to have much impact! As Carlo Dani suggests in this review there is no current evidence that clinically important outcomes are improved, but I am going to say something which is probably unique among the posts on this blog: I don’t think we need such evidence. I can’t see any downside to reducing episodic, or sometimes prolonged, hyperoxia and hypoxia in preterm infants, or indeed in infants at term either. As long as the devices actually work, and do adjust FiO2 to achieve more stable saturations and reduce episodes of desaturation followed by re-oxygenation, and episodes of excessively high saturations, that would be sufficient for me to buy them for every baby in the NICU. I can’t see how it could possibly be harmful, and it would probably reduce nurses stress and turnover and decrease parental stress also!
Manual adjustment of the FiO2 by the nursing staff (usually in response to alarms) has been shown in some of the studies to be substantially reduced by automated oxygen control (Hallenberger A, et al. Closed-loop automatic oxygen control (CLAC) in preterm infants: a randomized controlled trial. Pediatrics. 2014;133(2):e379-85).
Many times parents become stressed when their baby’s alarms ring, the most common alarm, by far, is from the pulse oximeter, and when the nurse doesn’t come immediately (most often when there is a minor desaturation or high sat alarm and the nurse knows from experience of that baby that just waiting a little while will correct the saturation) they can sometimes freak out. The extra reassurance that there is a device active which is regulating the oxygen requirements will help a little to reduce the stress of having a baby in intensive care.








