As well as all the high tech mechanistic studies in NEC, such as those that I just posted about, sometimes we need to take a step back and ask some very basic questions. What is the current natural history of NEC? How good are we at diagnosing NEC?
So much has changed in neonatology since NEC was first described, that this new study from the Pediatrix database is timely, (Mara K, et al. Necrotizing Enterocolitis in Very Low Birth Weight Neonates: A Natural History Study. Am J Perinatol. 2022). It includes data from babies born 23 to 29 weeks GA who had a birthweight less than 1500g. The babies were divided into those with suspected, medical or surgical NEC. It shows a peak in confirmed NEC incidence around 2007, with a fairly marked decrease since then, being relatively stable since 2015. There has also been a switch in antibiotics used, with much more Piperacillin/Tazobactam, much less 3rd generation cephalosporins, and a drop in vancomycin use over the last few years. There has also been a switch from clindamycin to metronidazole for anaerobic coverage.
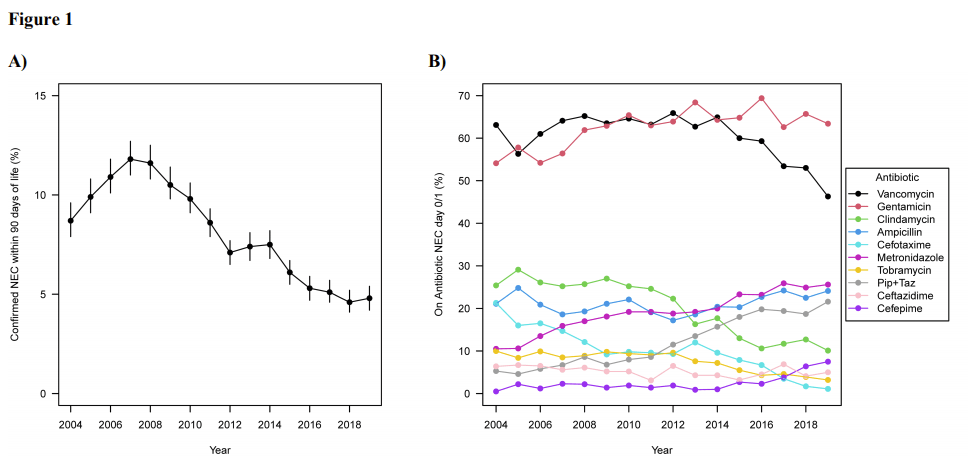
There is a huge amount of data in this publication, so I will just mention a few highlights. Risk factors for development of NEC are confirmed as being lower GA, male sex, small for gestational age and being outborn. Mortality is elevated, and is extremely high for surgical NEC: 6% for suspected NEC, 16% for medical NEC and 43% for surgical NEC. Positive blood cultures within 7 days of diagnosis were positive in 20%, and among surgical NEC were positive in 40%. Postnatal growth restriction was common among these babies, especially the surviving surgical NEC infants.
In addition to the obvious human costs of NEC the calculated additional financial costs are enormous. Length of stay was 26 days longer for confirmed NEC babies, and just on that basis average increased hospital charges are about $200,000 per case. Which can be calculated for the whole of the USA to be nearly half a billion dollars a year. That estimate does not include post-discharge costs, which are also enormously increased for NEC babies. Any intervention which has a reasonable cost and which decreases NEC will save money, as well as lives. Another good reason for funding NEC research!
The study has the advantages and limitations of a large database, meaning that individual diagnoses were not verified (of course) and we have to assume that these were all cases of NEC. That assumption is challenged somewhat by this meticulous individual examination of cases; BErrington J, Embleton ND. Discriminating necrotising enterocolitis and focal intestinal perforation. Arch Dis Child Fetal Neonatal Ed. 2022;107(3):336-9. By examining in detail the case records of babies in their local database, it was clear that differentiating the 2 phenomena is difficult, there is overlap in age of presentation, clinical signs at presentation, complications and outcomes. There is even confusion when the histology is examined. Only by really carefully examining each individual case were they able to come up with a final decision, and I am sure they would agree that other people examining the same cases might sometimes have different conclusions! Spontaneous intestinal perforation, with the typical anti-mesenteric perforation in the absence of skip necrotic lesions, has some aetiologic characteristics in common with NEC, but I think it is unlikely that interventions to prevent NEC will also prevent SIP.
The long term outcome impacts of NEC are well known, the data about SIP outcomes are more inconsistent, but there do appear to be substantial adverse impacts on neurological outcomes and on developmental progress. There are also major impacts of NEC on feeding and nutritional outcomes, and associations with lung injury and retinopathy and behavioural problems.
On this day we need more than just awareness, a co-ordinated effort to reduce the incidence and the impact of NEC, and SIP, will improve the future lives of thousands of babies and their families.









Dear Keith, thanks for your NEC awareness call! I completely agree regarding the problem of diagnosis of NEC. Probably, some “NEC-cases” even have a Food Protein Induced Allergic Enterocolitis (FPIAP). Over the last decade, we gradually changed the management of neonates with bloody stools at our institution. Except for neonates undergoing surgery, we still don’t know which one has NEC and which one has FPIAP, but we were able to reduce the overtreatment of neonates for suspected NEC. Our small retrospective study has major limitations, but it may be a small hint that not every neonates with bloody stool, even with pneumatosis coli, has NEC and need PEN and antibiotics (https://pubmed.ncbi.nlm.nih.gov/34943679/).